A Doctor Explains Why Ovarian Cancer Is So Difficult to Catch Early
Ovarian cancer is often referred to as “the silent killer” for a good reason: It ranks as the fifth deadliest cancer among women. In fact, of the 22,530 women who will receive an ovarian cancer diagnosis each year, nearly 14,000 of them will die from it, according to the American Cancer Society (ACS).
One big reason for that: Ovarian cancer is difficult to catch. A combo of factors—from lack of screening to easily-ignored symptoms—can result in a later-stage diagnosis, when the cancer has progressed beyond the ovaries.
That’s why understanding your risk is so important. In addition to a family history and simply getting older, a number of factors can increase the odds of developing this deadly cancer. Here’s what one leading expert wants women to know about ovarian cancer symptoms, why it can be so dangerous, and how to identify and monitor your health.
What all women should know about ovarian cancer
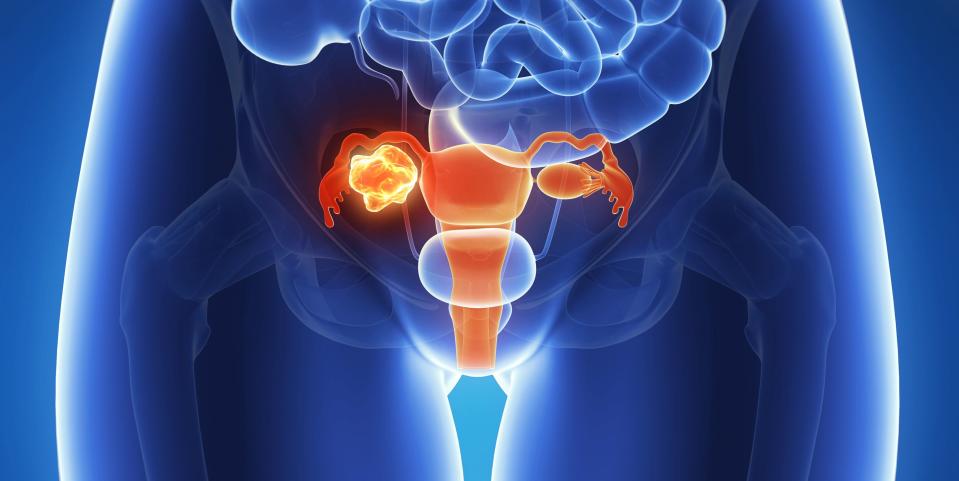
Ovarian cancer, which affects the two almond-sized glands that produce a woman’s reproductive hormones (like estrogen) and eggs, is one of a few gynecological cancers women potentially face. Of the three types of ovarian cancer, which involve different types of tumors, the most common cancer is caused by epithelial tumors, which grow in the tissue that covers the outside of the ovaries.
“With about 22,000 to 23,000 new cases of ovarian cases in the U.S. per year, it’s the second most common gynecological cancer,” explains Konstantin Zakashansky, MD, a gynecologic oncology specialist at Mount Sinai Hospital in New York City. (Endometrial cancer is about twice as common—and, no, gynecological cancers do not include breast cancer.)
But while ovarian cancer is less common than endometrial cancer, it causes far more deaths, according to the U.S. National Library of Medicine. In fact, according to Dr. Zakashansky, upwards of 70 percent of ovarian cancer cases aren’t diagnosed until stage three or four, when it has spread beyond just the ovaries. Meanwhile, most cases of endometrial cancers are diagnosed in earlier stages.
So, why is ovarian cancer so hard to diagnose?
While endometrial cancer may cause bleeding as it develops, ovarian cancer develops much more quietly—hence why it’s called “the silent killer.”
But research shows that most women with ovarian cancer were seeing their doctor about symptoms for more than six months before they received a diagnosis.
One major reason for the delay: Ovarian cancer develops deep within the lower abdomen, resulting in symptoms that are as non-specific as they get. Bloating, abdominal discomfort, indigestion, and frequent urination are all signs of ovarian cancer—but they’re also signs of eating too much, food allergies, general GI issues, or even a urinary tract infection, which are all much more common than cancer. (Read about how one woman’s weight gain and nagging heartburn led to her diagnosis.)
As a result, “most patients with ovarian cancer don’t get a diagnosis until the mass is really big,” Dr. Zakashansky says, meaning it will only become more difficult to treat successfully.
And while other types of cancer spread to various organs (like prostate cancer, which often spreads to the lungs), ovarian cancer typically stays within the abdominal cavity, which further delays detection, explains Dr. Zakashansky.
Another issue? There aren’t any early detection screening tests for ovarian cancer—like the mammogram all women are urged to get every year once they turn 45—despite ongoing research, the ACS says. Ultimately, ovarian cancer is diagnosed after an ultrasound or CT scan identifies abnormal growths and either a blood test or biopsy confirms the growth to be cancerous.
Understanding your ovarian cancer risk
A few factors increase a woman’s risk of ovarian cancer, including:
Age (half of all ovarian cancers are found in women 63 or older)
Genetic mutations
Family history
Early menstruation, later menopause, or both
Not bearing children
According to Dr. Zakashansky, about 20 percent of women have one or more of the 20 genetic mutations that can increase risk of certain cancers, including the BRCA1 and BRCA2 genes.
Additionally, having an immediate family member (like your mother, grandmother, or aunt) who’s been diagnosed with breast cancer or any gynecological cancer also increases your risk of ovarian cancer, even if you don’t have one of those genetic mutations.
If you have a family history of any of these cancers, Dr. Zakashansky recommends talking to your doctor about doing genetic testing to identify any mutations. Women with both genetic mutations and family history are considered high-risk patients, and should see their doctor every six months for screenings, which typically include pelvic exams, ultrasounds, and blood tests to identify proteins often present in cancer.
If you experience symptoms like abdominal pain, bloating, frequent urination, constipation, an upset stomach (like nausea and vomiting), and irregular bleeding that can’t otherwise be explained, talk to your doctor about the possibility of ovarian cancer, says Dr. Zakashansky. The earlier you reach a diagnosis, the earlier you can start potentially life-saving treatment.
Like what you just read? You’ll love our magazine! Go here to subscribe. Don’t miss a thing by downloading Apple News here and following Prevention. Oh, and we’re on Instagram too.
You Might Also Like
